HER+ Fight with Cancer
Ruth was 79 years old when she was diagnosed with early stage I breast cancer in 2018. A breast lump had been found on a routine examination.
A biopsy later confirmed breast cancer. Further testing confirmed that the surface of her cancer cells was covered with a protein called HER2. The presence of HER2 protein on the cancer cells indicated a more aggressive form of breast cancer with a higher recurrence rate. Fortunately, there was an effect therapy for HER2+ breast cancer. Ruth’s oncologist wanted her to receive Herceptin (trastuzumab), an immune therapy shown to improve survival and decrease cancer recurrence. After undergoing a lumpectomy to remove the cancer, her oncologist prescribed treatment with from Herceptin and Taxol, a chemotherapeutic agent.
Before starting Herceptin, Ruth had an echocardiogram, which is an ultrasound study to evaluate the heart pump function. Unfortunately Ruth’s echocardiogram showed that her heart heart function was moderate to severely reduced. One of the potential side effects of Herceptin was a weakening of the heart pump, which can cause congestive heart failure. She was therefore referred to the 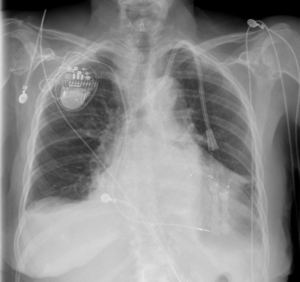 Cardio-Oncology Clinic at MHVI. Ruth’s cardiologist decided that she could improve her heart function with the use of a special pacemaker, called a biventricular pacemaker. This pacemaker was designed to improve heart function in patients with a low heart function and certain electrical conduction defects. A biventricular pacemaker was successfully placed in Ruth (see x-ray). A follow-up echo showed that her ejection fraction had improved enough to start treatment with Herceptin. She was followed closely in the Cardio-Oncology Clinic while receiving cancer treatment and in the end completed 6 months of therapy with Taxol and Herceptin with no signs of additional weakening of the heart function. Throughout her course of chemotherapy, Ruth was able receive cancer treatment with minimal damage to her heart. Now, more than two years later she is doing well. Ruth is able to play with her grandkids, attend church, and she remains cancer-free.
Cardio-Oncology Clinic at MHVI. Ruth’s cardiologist decided that she could improve her heart function with the use of a special pacemaker, called a biventricular pacemaker. This pacemaker was designed to improve heart function in patients with a low heart function and certain electrical conduction defects. A biventricular pacemaker was successfully placed in Ruth (see x-ray). A follow-up echo showed that her ejection fraction had improved enough to start treatment with Herceptin. She was followed closely in the Cardio-Oncology Clinic while receiving cancer treatment and in the end completed 6 months of therapy with Taxol and Herceptin with no signs of additional weakening of the heart function. Throughout her course of chemotherapy, Ruth was able receive cancer treatment with minimal damage to her heart. Now, more than two years later she is doing well. Ruth is able to play with her grandkids, attend church, and she remains cancer-free.
Ruth’s story highlights one of the main goals of the Cardio-Oncology Clinic at MHVI. We work closely with cancer patients and their cancer specialists to help patients receive optimal cancer therapy while trying to prevent or minimize cancer related heart toxicity and symptoms.
>> Learn more about Cardio-Oncology Clinic
>> Learn more about Biventricular Pacemaker (Cardiac Resynchronization Therapy)



Leave a Reply
Want to join the discussion?Feel free to contribute!